Chemotherapy-induced hypersensitivity
exp date isn't null, but text field is
There is no universally agreed definition of anaphylaxis and the following definition is offered by the European Academy of Allergology and Clinical Immunology Nomenclature Committee: ‘Anaphylaxis is a severe, life-threatening, generalised or systemic hypersensitivity reaction’. This is characterised by rapidly developing lifethreatening airway and/or breathing and/or circulation problems usually associated with skin and mucosal changes (Resuscitation Council - 2008)
Anaphylactic Response:
- A hypersensitivity reaction can occur when the immune system is provoked by an antigen such as a cytotoxic drug, stimulating the formation of certain IgE antibodies that attach to receptors on mast cells and basophils. A subsequent exposure to the same antigen will trigger these antibodies, causing degranulation of the cell and thereby releasing chemical mediators such as histamine, serotonin, slow-reacting substance of anaphylaxis (SRS-A), and eosinophil chemotactic factor of anaphylaxis (ECF-A). When released from cells into the circulatory system, the chemical mediators produce an anaphylactic response.
- Anaphylactoid reactions differ from anaphylactic reactions in that no prior exposure to the agent is necessary to induce the response. The agent itself, not the IgE antibodies, will bind directly to the surface of the cells, causing direct degranulation and a release of mediators. Anaphylactoid and anaphylactic reactions have identical signs and symptoms and are treated in the same manner.
- Anaphylaxis is a severe, rapid, systemic and life threatening allergic reaction that presents as a medical emergency. It can be precipitated in susceptible individuals by a wide range of substances, however, for the purpose of this document, the substances are cytotoxic drugs and biological therapies. Anaphylaxis requires rapid recognition, treatment and management by health professionals.
- Cancer chemotherapy drugs are foreign substances capable of inducing anaphylaxis and reactions which range from mild cutaneous symptoms to severe respiratory distress and cardiovascular collapse. This adverse/allergic reaction can occur within seconds or minutes of drug administration with features of an anaphylactic reaction. Nurses need to be aware of the signs and symptoms of such reaction because if doctors are not immediately available, nurses are responsible for not only recognising the symptoms of a hypersensitivity reaction, but also for treating it promptly.
All health care professionals should understand the causes of anaphylaxis, know how to diagnose anaphylaxis and be able to administer effective treatment.
None.
Any member of qualified medical staff or Advanced Nurse Practitioner can investigate and manage patients with chemotherapy-induced hypersensitivity.
None.
5.1 Recognition of an Anaphylactic Reaction
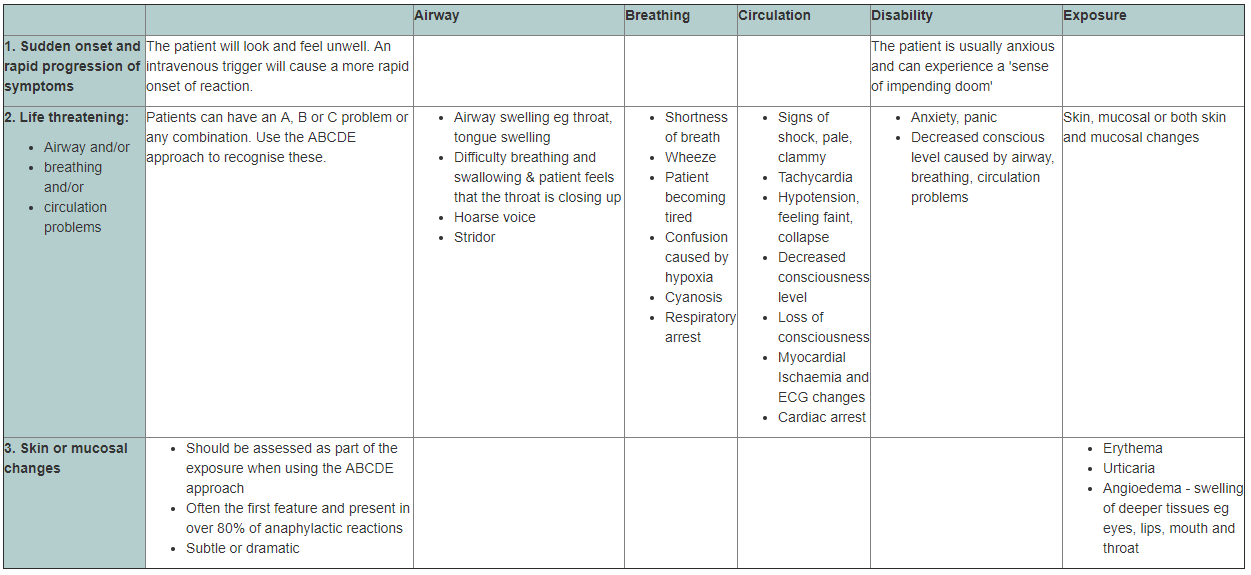
A diagnosis of an anaphylactic reaction is likely if a patient who is exposed to a trigger (allergen) develops a sudden illness, usually within minutes of exposure, with rapidly progressing skin changes and life-threatening airway and/or breathing and/or circulation problems. The reaction is usually unexpected.
The range of signs and symptoms vary and certain combinations of signs make the diagnosis of an anaphylactic reaction more likely. When recognising and treating an acutely ill patient, a rational ABCDE, Airway, Breathing, Circulation, Disability (relating to patients conscious level), Exposure (relating to skin and mucosal changes) approach must be followed and life-threatening problems treated as they develop - see Appendices.
5.2 Differential Diagnosis
Life threatening conditions
- Asthma – can present with similar symptoms and signs to anaphylaxis, particularly in children
- Septic Shock – hypotension, usually in association with a temperature > 38C or < 36C. There is an increased risk if central venous access has been used recently
Non life threatening conditions
- Vasovagal episode
- Panic attack
- Breath holding in a child
- Idiopathic (non-allergic) urticaria or angioedema
Seek help early if there are any doubts about the diagnosis.
5.3 Education
Anaphylaxis can be fatal and therefore healthcare workers require regular training in recognising, treating and managing anaphylaxis.
Patients should be given appropriate information and education to enable them to identify signs of chemotherapy-induced anaphylaxis and emphasise the need to report these signs immediately if the occur.
|
Action |
Rationale |
|
Identify patients at increased risk of chemotherapy induced anaphylaxis by taking a full history of previous allergic reactions |
To identify patients at risk of allergic reaction thus anaphylaxis thus minimising risk |
|
Provide the patient with appropriate information and education to enable them to identify signs of chemotherapy induced anaphylaxis and emphasise the need to report these signs immediately if they occur |
To allow early detection and intervention minimising adverse effects |
|
Ascertain if any pre-treatment steroids have been taken; or are to be administered prior to chemotherapy |
To identify concurrent measures that may or may not be required if a chemotherapy induced anaphylactic reaction occurs (i.e. has the patient had dexamethasone as part of pre-chemotherapy anti-emetic) |
|
Prior to administration of chemotherapy, nursing/medical staff should be familiar with the likelihood of the drug causing anaphylaxis and have easy access to emergency equipment and drugs |
To allow early detection and minimising adverse effects
|
ANY DRUG CAN CAUSE IMMEDIATE HYPERSENSITIVITY REACTIONS
Management of a Mild to Moderate Acute Hypersensitivity Reaction or Allergic Reaction:
Mild to moderate Adverse Drug Reaction – slowly progressing peripheral oedema or changes restricted to the skin eg urticaria.
|
Action to be taken |
Rationale |
|
1. Stop the infusion/injection of chemotherapy immediately, maintaining IV access |
To prevent further exposure to the allergen and minimise any further adverse reaction |
|
2. Explain all care to the patient and their family |
To inform patient of what is happening and to help reduce anxiety |
|
3. Assess the patient's airway, breathing and circulation, and level of consciousness |
To ensure patient is not developing a more severe reaction |
|
4. Initiate frequent vital signs including oxygen saturation |
To monitor hypotension, tachycardia and respiratory status |
|
5. Recline the patient into a comfortable position |
May be helpful for patients with hypotension, however, may be unhelpful for patients with breathing difficulties |
|
6. Summon medical and nursing assistance |
Ensures prompt support especially if patient's condition deteriorates |
|
7. Never leave the patient alone |
Risk of shock/severe reaction |
|
8. Administer Chlorphenamine (IM or slow IV):
NB –repeat for all as necessary to a maximum of 4 doses per day |
Counter histamine mediated vasodilation |
|
9. Administer hydrocortisone (IM or slow IV):
NB –all above should be adjusted according to response |
|
|
10. Document allergic reaction fully in the medical and nursing notes |
Prevention |
|
11. Monitor for 8 - 24 hours |
Risk of early recurrence |
|
12. Treat prophylactically for the next treatment |
Prevention |
Management of Anaphylaxis:
Anaphylaxis with cardiovascular collapse – common manifestation, vasodilation and loss of plasma from blood compartment
|
Action to be taken |
Rationale |
|
13. Call the cardiac resuscitation team and commence CPR if necessary |
|
|
14. Recline the patient into a comfortable position |
May be helpful for patients with hypotension, however, may be unhelpful for patients with breathing difficulties |
|
15. Administer oxygen 10 - 15L/min |
To increase cell perfusion |
|
16. Administer Adrenaline 1:1000 solution to 0.5mL (500 micrograms) IM
|
Alpha-receptor agonist, it reverses peripheral vasodilation and reduces oedema. Its beta-receptor activity dilates the airways, increases the force of the myocardial contraction and suppresses histamine and leukoytriene release |
|
17. Administer Chlorphenamine (IM or slow IV):
NB –repeat for all as necessary to a maximum of 4 doses per day |
Counter histamine mediated vasodilation |
|
18. Administer hydrocortisone (IM or slow IV):
NB –all above should be adjusted according to response |
|
|
19. Repeat dose of Adrenaline only after 5 minutes and if no clinical improvement |
Recovery can be transient and sometimes several doses may be required |
|
20. If severe hypotension does not respond rapidly to drug treatment, IV fluids 10ml/kg, 0.9% saline |
Improve hypotension |
|
21. Record vital signs and maintain accurate documentation |
|
|
22. Obtain clotted blood 45 - 60 minutes after and no later than 6 hours, for specific IgE antibody and mast cell tryptase |
To assess whether episode is a genuine anaphylactic reaction |
|
23. Admit patient |
Repeat episode can occur 1-72 hours after clinical recovery |
Other Concurrent Measures:
|
Action |
Rationale |
|
1. If bronchospasm severe and does not respond to other treatment - administer Salbutamol |
To reduce bronchospasm |
|
2. Provide support to the patient and their family. Display a calm, competent and confident disposition. Reassure and explain to the patient and any relatives what is being done and what should be expected to happen shortly. |
To reduce patient anxiety and promote wellbeing, by educating patients on delayed side effects and how to deal with them in the first instance. |
|
3. Ensure the episode is accurately documented (to include sensitivity) in appropriate nursing and medical records. |
To meet legal requirements and prevent/minimise future problems. |
Adult Chemotherapy Induced Anaphylaxis Policy (Beatson West of Scotland Cancer Centre, April 2010)
Last reviewed: 01 November 2021
Next review: 01 November 2023
Author(s): Dr Dermot Murphy
Version: 2
Approved By: Sch Clin Gov Group
Document Id: RHC-HAEM-ONC-033