In most babies, laryngoscopy results in a clear view of the larynx. However, this is not always the case. The view of the larynx is classified as follows (3):
- Grade 1 – visualisation of the entire laryngeal aperture. There should be little difficulty with intubation.
- Grade 2 – visualisation of the posterior portion of the laryngeal aperture. There may be some difficulty passing the ETT. We can attempt to improve this view by applying ‘cricoid’*.
- Grade 3 – only the epiglottis can be visualised. This can result in severe difficulties. Cricoid/ BURP may help visualisation.
- Grade 4 – only visualisation of the soft palate is possible. Intubation is always difficult and usually accompanies obvious pathology but may also occur unexpectedly (Figure 1).
Figure 1: Laryngoscopy views
* By ‘cricoid’ we actually mean ‘BURP’ which stands for applying Backwards, Upwards, Right Pressure to the larynx. Cricoid in the truest sense of the word means compression of the oesophagus to prevent aspiration.
Figure 2: ‘BURP’
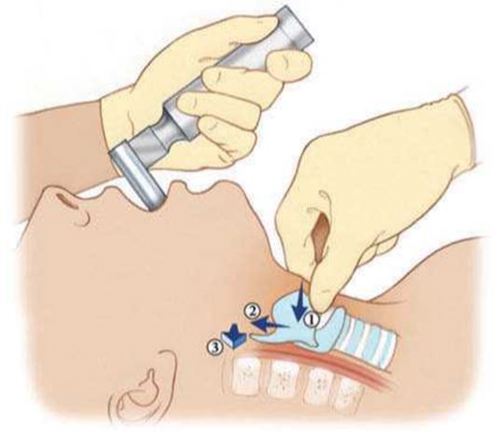 |
1 - ‘Backward’ pressure towards cervical spine 2 - ‘Upward’ pressure towards jaw 3 - ‘Right pressure’ – push larynx towards baby’s right. |