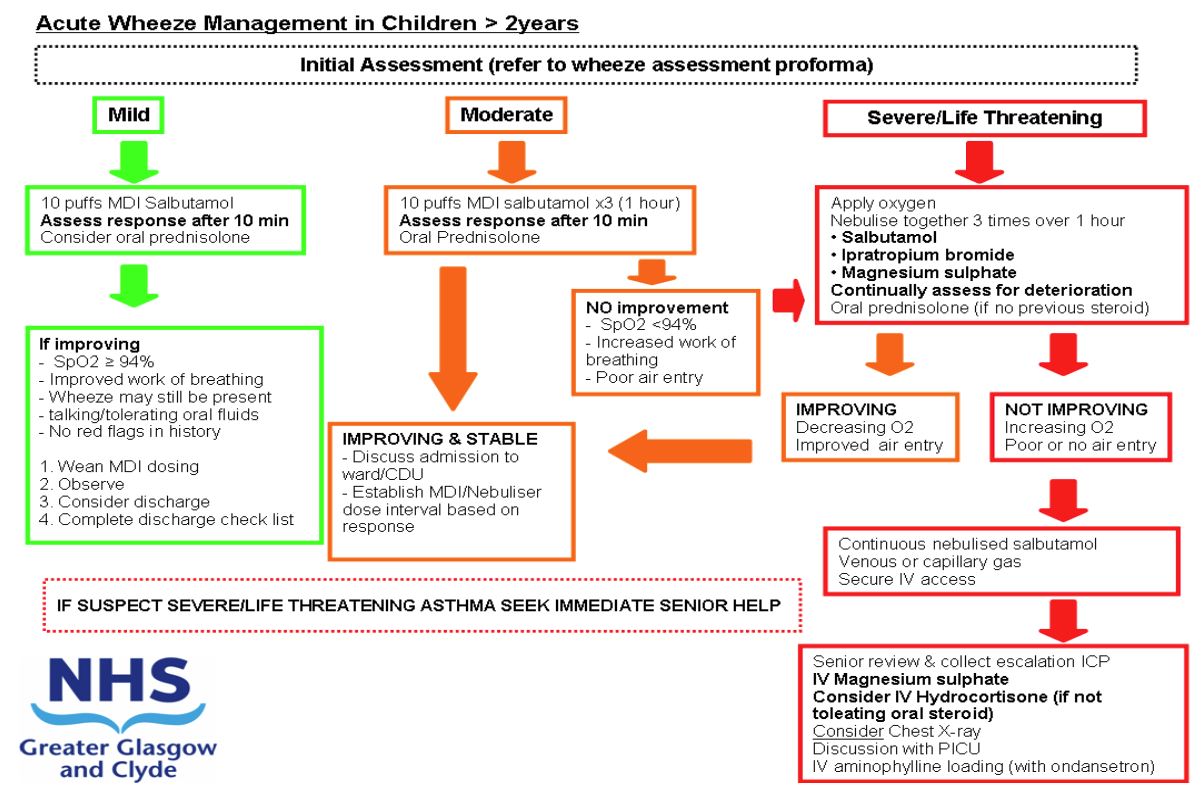
Acute wheeze in children 2 years and older: assessment and management
exp date isn't null, but text field is
Objectives
This guidance replaces the previous guidelines "Acute asthma in children aged between 2 and 5 years" and "Acute asthma in children > 5 years"
Separate guidance is available for Acute asthma in children aged < 2 years.
November 2023: This guidance is currently under review as it has gone beyond the standard review date. It reflects best practice at the time of authorship / last review and remains safe for use. If there are any concerns regarding the content then please consult with senior clinical staff to confirm.
|
MILD AND
|
MODERATE AND
|
|
SEVERE AND
|
LIFE THREATENING AND
|
- Has the patient previously received IV therapy for wheeze management?
- Has the patient been admitted to the PICU previously for respiratory illness?
If YES to any of the above then patient should be discussed with on call Paediatric Registrar prior to discharge.
Salbutamol MDI + Spacer – Initial therapy = 10 puffs. (100mcg per puff)
Oxygen – minimum 6 l/min via non-rebreather mask
| Prednisolone |
|
2 -4yrs 20mg OD >5yrs 40mg OD |
| Nebulised medication for Severe Wheeze | |
|
2 -4yrs |
Salbutamol 2.5mg |
| >5yrs |
Salbutamol 5mg |
IV MEDICATION
(To be prescribed as per the Escalation to IV therapy care pathway)
| 1. Magnesium sulphate injection |
40mg/kg over 20 minutes (max 2gram) |
||||
|
2. Aminophylline |
|
||||
|
3. Salbutamol |
|
||||
|
- Hydrocortisone - Ondansetron |
4mg/kg QDS (max 100mg) 100micrograms/kg (max 4mg) |
- Patient maintaining saturations > 94% in air
- Tolerating 3hrly multidosing
|
Patients with MILD asthma at 1st assessment can be discharged after Salbutamol without being monitored for 4 hours |
- Discharge Checklist Completed
- No red flag features
- If presenting with interval symptoms medication reviewed and consideration given to starting Clenil Modulite 100mcg BD
- Follow-Up arranged as below
- BTS/SIGN British guideline on the management of Asthma; 2019.
- Mechanism of lactic acidosis in children with acute severe asthma; Meert KL, McCaulley L, Sarnaik AP. Paediatric Critical Care Medicine. 2012 Jan;13(1):28-31
- A Clinical Guideline for the use of Aminophylline in Acute Severe Asthma in Children; Norfolk and Norwich University Trust. Dr Caroline Kavanagh; 5th April 2017
- Aminophylline Dosage in Children Asthma Exacerbations in Children: A Systematic Review; Cooney L, Sinha I, Hawcutt D. PLoS One. 2016.
- Standards for Level of Asthma Intervention; Greater Glasgow and Clyde Health Board
- Aminophylline Hydrate; December 2015.
- BNF for Children. Aminophylline.
- BNF for Children. Hydrocortisone
- BNF for Children. Prescribing for children: weight, height and gender.
- Clinical Practice Guidelines: Asthma Acute. The Royal Hospital for Children, Melbourne. May 2015
Last reviewed: 11 June 2020
Next review: 31 October 2024
Author(s): Dr Steve Foster (Consultant in Paediatric Emergency – Paediatric Emergency Department), Dr Morag Wilson (Consultant in General Paediatrics – Acute Paediatrics)
Approved By: Clinical Effectiveness
Document Id: 623